Contents
- What is Loperamide?
- Loperamide drug class
- How Loperamide works in the body?
- Loperamide brand names
- What is Loperamide used for?
- Loperamide dosage for different indications
- Loperamide side effects
- How to take Loperamide?
- Loperamide abuse and addiction
- Can loperamide make you ‘’high’’?
- Loperamide withdrawal
- Precautions and warnings during Loperamide use
- Can I take loperamide if I have abdominal pain without diarrhea?
- Can I take loperamide if I have infective diarrhea?
- How long does Loperamide take to work?
- How long loperamide stay in your system?
- Loperamide during pregnancy
- Loperamide during breastfeeding
- Can you give Imodium to a child?
- Loperamide overdose
- Can I drink alcohol while taking Loperamide
- Loperamide and simethichone combination
- Can loperamide cause paralytic ileus?
- Can loperamide cause electrolyte loss?
- Loperamide and Quinidine interaction
- Can I take loperamide and clarithromycin together?
- Can I take loperamide and diltiazem (Cardizem) together?
- Can I take loperamide and gemfibrozil (Lopid) together?
- Can I take loperamide and Plavix together?
- Can I take ranitidine and loperamide together?
- Can I take loperamide and spironolactone together?
- Is loperamide a controlled substance?
- Can I give Imodium to the dogs?
- Imodium and opiate withdrawal
- Precautions when using loperamide for opiate withdrawal
- Can I take loperamide and Pepto Bismol together?
- Can I take Loperamide and Tylenol together?
- Can I take Loperamide and Tums together?
What is Loperamide?
Loperamide is a Generic name for a long-acting synthetic antidiarrheal drug. This drug works by slowing intestinal motility via opioid receptor and has direct effects on circular and longitudinal muscle. It also reduces fecal volume and increases viscosity, making stool less watery. OTC loperamide is most commonly used to control diarrhea, including travelers’ diarrhea.
On the other hand, prescription loperamide is most commonly used for conditions such as: gastroenteritis, short bowel syndrome and IBC – inflammatory bowel disease. Prescription loperamide is also used to decrease the amount of fluid in patients with ileostomies. It is not recommended for patients who have blood in the stool and should not be used in children younger than 2 years of age. It may increase the risk of toxic megacolon.
Loperamide is probably best known as Brand name Imodium. Loperamide is available in a tablet, chewable tablet, capsule, and liquid form to take by mouth. It’s available with or without a prescription as capsule or tablet in dose of 2 mg and as a solution in doses of 1mg/5ml and 1mg/7.5ml.
It was first made in 1969 and used in medical purpose in 1976. It is on the WHO’s List of Essential Medicines one of the most effective and safe medicines needed in a health system.

Loperamide molecular formula and weight
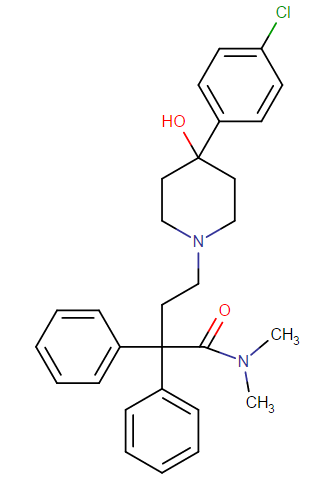
Loperamide Hydrochloride contains not less than 98 % and not more than 102 % of C29H33ClN2O2·HCl, calculated on the dried basis.
Loperamide IUPAC name is: 1-Piperidinebutanamide,4-(4-chlorophenyl)-4-hydroxy-N,N-dimethyl-a,a-diphenyl-,monohydrochloride.
Loperamide molecular formula is: C29H33ClN2O2·HCl
Loperamine molecular weight is: 477.045 g/mol
Loperamide drug class
Loperamide chemically belongs to the class of chemical compounds known as diphenylmethanes. These are molecules containing a diphenylmethane moiety, which consists of methane wherein two hydrogen atoms are substituted by two phenyl groups.
How Loperamide works in the body?
Loperamide is an agonist of opioid receptor that acts on the mu opioid receptors in the myenteric plexus of large intestines. It does not affect CNS like other opioids. It works specifically by reducing the activity of the myenteric plexus further decresing the motility of the circular and longitudinal smooth muscles of the intestinal wall.
This actions increase the amount of time food and other substances stay in the intestine, permitting for more water to be absorbed out of the fecal matter. Loperamide also lowers colonic mass movements and inhibits the gastrocolic reflex. In vitro studies showed that loperamide is non-selective calcium channel blocker and binds to opioid mu-receptors. Findings suggest that at higher concentrations loperamide binds to calmodulin.
Loperamide brand names
Probably most common brand name for loperamide is Imodium. Other Brand names for loperamide on the market are: Dimor, Fortasec, Kaopectate II, Lopedium, Lopex, Maalox Anti-Diarrheal.
What is Loperamide used for?
Loperamide is used most commonly for a short-term to control and symptomatic relief of acute nonspecific diarrhea and in some situations chronic diarrhea related with inflammatory bowel disease or gastroenteritis. It is also used in order to reduce the volume of discharge from ileostomies.
FDA approved indications for Loperamide are:
- Chronic Diarrhea
- Diarrhea
- Intestinal stoma leak
- Traveler’s Diarrhea
Loperamide dosage for different indications
Usual Adult Dose for Acute Diarrhea
Tablets, capsules, and liquid:
Initial: 4 mg (2 doses of 2mg) orally after the first loose stool, then
Maintenance: 2 mg after each loose stool. 16 mg in any 24-hour period should not be exceeded.
Chewable tablets:
Initial: 4 mg after the first loose stool, then
Maintenance: 2 mg after each subsequent loose stool, but not exceeding 8 mg in 24 hours.
Usual Adult Dose for Chronic Diarrhea
Tablets, capsules, and liquid:
Initial: 4 mg orally once followed by 2 mg orally after each loose stool. 16 mg in any 24-hour period should not be exceeded.
Maintenance: The average maintenance dosage is 4 to 8 mg by day. If clinical improvement is not observed at a maximum dosage of 16 mg during 10 days of treatment, symptoms are unlikely to be controlled by further administration.
Usual Pediatric Dose for Acute Diarrhea
2 to 6 years (13 to 20 kg):
Liquid formulation only to be used in this age group.
Initial: 1 mg orally 3 times per day for the first day, then
Maintenance: 0.1 mg/kg/dose after each loose stool, but not exceeding initial dose.
6 to 8 years (20 to 30 kg):
Tablets, capsules, and liquid:
Initial: 2 mg orally twice a day at first day, then
Maintenance: 0.1 mg/kg/dose after each loose stool, but not exceeding initial dose.
Chewable tablets:
Initial: 2 mg orally after the first loose stool, then
Maintenance: 1 mg orally after each subsequent loose stool, but not exceeding 4 mg in 24 hours.
8 to 12 years (greater than 30 kg):
Tablets, capsules, and liquid:
Initial: 2 mg orally 3 times a day for the first day, then
Maintenance: 0.1 mg/kg/dose after each loose stool, but not exceeding initial dose.
Chewable tablets:
Initial: 2 mg orally after the first loose stool, then
Maintenance: 1 mg orally after each subsequent loose stool, but not exceeding 6 mg in 24 hours.
12 to 18 years:
Tablets, chewable tablets, capsules, and liquid:
Initial: 4 mg after the first loose stool, then
Maintenance: 2 mg after each subsequent loose stool, but not exceeding 8 mg in 24 hours.
Less than 2 years:
Loperamide should not be used in children younger than 2 years of age,
Loperamide side effects
Loperamide may cause following side effects:
- Dizziness
- Fatigue
- Abdominal pain
- Constipation
- Nausea
- Dry mouth
- Angioedema
- Bullous eruptions
- Flatulence
- Rash
- Pancreatitis
- QT/QTc interval prolongation, Torsades de Pointes, other ventricular arrhythmias, cardiac arrest, syncope, and death
Adverse effects most commonly associated with loperamide are: constipation occuring in 1.7–5.3% of users, dizziness occurring up to 1.4%, nausea with a rate of 0.7–3.2% and abdominal cramps 0.5–3.0%.
Rare, but very serious side-effects during loperamine use may include: paralytic ileus, toxic megacolon, angioedema, anaphylaxis/allergic reactions, Stevens-Johnson syndrome, toxic epidermal necrolysis, erythema multiforme, urinary retention, and heat stroke
How to take Loperamide?
Always take loperamide as directed by your doctor. Check the label on the medicine for exact dosing instructions.
- You can take loperamide by mouth with or without food.
- Drinking extra fluids is recommended while you have diarrhea. Check with your doctor if you have questions.
- If you miss a dose of loperamide, take it as soon as you remember. Continue to take it as directed by your doctor or on the package label.
Ask your health care provider any questions you may have about how to use loperamide.
Loperamide abuse and addiction
Studies found that when Loperamide is used at high doses findings were that it had extremely low abuse potential.
Studies in monkeys who were morphine-dependent demonstrated that loperamide at doses above those recommended for humans use was effective in preventing symptoms of morphine withdrawal. However, in humans, the pupil test indicating opiate-like effects, performed after a single high dose or after long-term loperamide use was negative.
Orally administered loperamide formulated is both highly insoluble and penetrates the CNS poorly. It has been also concluded that in the form of capsules, when mixed with magnesium stearate, loperamide poses little threat of potential abuse. Many of the users report that Loperamide helped them, somewhat successfully, to treat opiate withdrawal symptoms.
Can loperamide make you ‘’high’’?
There are reports that taking very high doses of 100 mg of loperamide per day may achieve a euphoric affect, however this doses are never recommended. The reported experience is not nearly as intense after narcotic painkillers use, but it lends a sense of overall well-being.
To take enough of loperamide in order to reach any kind of “high” effect, it should be taken farm over the recommended daily amount, which may provoke lots of discomfort and harm, and serious side effect such as paralytic ileus.
Common adverse reactions associated with taking high doses of loperamide will include constipation, abdominal pain and bloating, nausea, vomiting. Rare reports associated with loperamide are dizziness, rashes and bowel obstruction.
Loperamide withdrawal
Withdrawal symptoms may occur after loperamide long-term use and discontinuation. There are, indeed, reports of experiences of opiate-like withdrawal including: sweats, cramps, shakes, diarrhea, and muscle aches have been reported following abrupt discontinuation of long-term therapy with loperamide.
Precautions and warnings during Loperamide use
- Patients should tell their doctor or pharmacist if they are allergic to loperamide or any other drugs, or any of the inactive ingredients in loperamide products. Always check the package label for a list of the ingredients.
- The use of loperamide is never recommended in patients with possible risk of significant sequelae such as ileus, megacolon, and toxic megacolon. Loperamide should be abrupted immediately in patients who develop constipation, abdominal distention, or ileus.
- There are some reports of toxic megacolon in patients with AIDS with infectious colitis viral and bacterial, treated with loperamide. Hence, loperamide therapy should be discontinued in AIDS patients at the first sign of possible abdominal distention.
- Patients should tell their doctor or pharmacist what other prescription and nonprescription medications, nutritional supplements, vitamins and herbal products you are taking or plan to take. They should mention if they are already using following drugs: antibiotics such as erythromycin (E.E.S., Ery-Tab, Eryc, others) and clarithromycin (Biaxin, in PrevPac), certain antifungals drugs such as itraconazole (Onmel, Sporanox) and ketoconazole; quinine (Qualaquin), quinidine (in Nuedexta), ritonavir (Norvir, in Kaletra), cimetidine (Tagamet), gemfibrozil (Lopid); ranitidine (Zantac), or saquinavir (Invirase). Doctor may need to adjust the doses of your medications or monitor you carefully for side effects.
- Patients should tell their doctor or pharmacist if they have a fever, black stools, blood or mucus in the stool, or difficulty swallowing.
- Patients should also tell their doctor or pharmacist if anybody in their family has or has ever had a prolonged QT interval (heart problem that may provoke irregular heartbeat, fainting, or sudden death) or any form of irregular heartbeat.
- Patients should tell their doctor or pharmacist if they have or ever had some liver disease.
- Patients should tell their doctor and pharmacist if they are pregnant or plan to become pregnant, or are breastfeeding. If you become pregnant while taking loperamide, call your doctor.
- Loperamide can make you drowsy and dizzy. Do not drive a car or operate machinery until you know how this drug affects you.
- Fluids and electrolytes should be replaced as needed.
Can I take loperamide if I have abdominal pain without diarrhea?
Loperamide is contraindicated in patients with abdominal pain that have no diarrhea. It is also not recommended as primary therapy in patients with acute dysentery with signs and symptoms such as blood in the stools and high fever, bacterial enterocolitis caused by invasive organisms including Shigella, Salmonella and Campylobacter, acute ulcerative colitis and in patients with pseudomembranous colitis caused by broad-spectrum antibiotics.
Can I take loperamide if I have infective diarrhea?
The use of drugs with antiperistaltic activity such as loperamide is contraindicated in patients with diarrhea caused by pseudomembranous enterocolitis or enterotoxin-producing bacteria. These drugs may prolong or even worsen diarrhea related with bacteria that invade the intestinal mucosa, such as toxigenic E. coli, Shigella, Salmonella, but also the pseudomembranous colitis caused by broad-spectrum antibiotics.
Other symptoms and complications such as fever, extraintestinal illness, shedding of organisms may also be increased or prolonged. Because antiperistaltic agents such as loperamide decrease gastrointestinal motility, excretion of infective gastroenteric organisms or toxins may be delayed thus it should be used cautiously in patients with any infectious diarrhea, particularly if accompanied by high fever or blood in the stool.
How long does Loperamide take to work?
In most uncomplicated cases 1-2 doses of loperamide will stop the diarrhea. So, benefits can be expected even after 1-2 hours of administration. However, clinical improvement is usually observed within 48 hours. Most commonly, this should be enough to stop acute diarrhea. For chronic diarrhea clinical improvement should be expected within 10 days.
How long loperamide stay in your system?
Studies showed that elimination half-life time of Loperamide in about 10.8 hours with a range of 9.1 to 14.4 hours. Plasma levels of loperamide are highest approximately 5 hours after taking the capsule and 2.5 hours after solution is taken. The peak plasma levels of Loperamide were similar for both formulations. Elimination of Loperamide mainly occurs by.
Cytochrome P450 (CYP450) isozymes oxidative N-demethylation . CYP2C8 and CYP3A4, are thought to play an important role in Loperamide metabolism. Furthermore, CYP2B6 and CYP2D6 appear to play a minor role in Loperamide N-demethylation. Elimination of the unchanged Loperamide and its metabolites usually occurs via the feces.
Loperamide during pregnancy
Loperamide has been assigned to pregnancy category C by the FDA pregnancy list of drugs. Animal studies have failed to find the evidence of teratogenicity or fetal harm. There are no controlled data in human pregnancy. Loperamide should only be given during pregnancy if the potential benefits outweigh the risks.
Loperamide during breastfeeding
Loperamide is can pass into human milk in small amounts. The effects in the nursing infant are still unknown. According to the manufacturer, loperamide should not be used during lactation
Study showed that loperamide was detected in the milk in six women taking loperamide oxide 4 mg orally two times a day for 2 doses. It has been estimated the ingested dose of loperamide in infants would be 2000 times less than the usual therapeutic dose. The infants did not breast-feed in this study.
Can you give Imodium to a child?
The use of loperamide in children under 2 years is contraindicated because of the increased risk of respiratory and cardiovascular side effects. There have been very rare reports of fatal paralytic ileus related with abdominal distention. Most of these reports occurred in acute overdose, and with very young children who have two years of age.
A review of loperamide use in children younger than 12 years of age found that serious side events occurred only in children under 3 years old. The study reported that the use of loperamide should be contraindicated in children under 3 years old, but also in patient who are systemically ill, moderately dehydrated, and malnourished or have bloody diarrhea. In 1990, in Pakistan all formulations for children of the antidiarrheal loperamide were banned in Pakistan.
Loperamide overdose
Maximum daily dose of loperamide is 16 mg. If more than 16 mg of loperamid is taken, overdose related side effects including following may happen:
- nausea
- inability to urinate
- fainting
- fast, pounding, or irregular heartbeat
- unresponsiveness
In cases of loperamide overdosage paralytic ileus, urinary retention and CNS depression may occur. Children are usually more sensitive to CNS side effects than adults. Clinical trials have showed that slurry of activated charcoal taken promptly after loperamide ingestion can reduce the amount of drug and be very effective for absorption inhibition.
If vomiting occurs spontaneously after administration, 100 gms of activated charcoal should be administered orally as soon as fluids can be retained. If vomiting didn’t occur, gastric lavage should be performed followed by administration of 100 gms of the activated charcoal through the gastric tube. Patients should be monitored for signs of CNS depression for at least 24 hours.
If overdose symptoms occur, naloxone can be given as effective antidote. If responsive to naloxone, vital signs must be monitored carefully for monitoring recurrence of symptoms during 24h.
Since relatively small amount of drug is excreted in the urine, forced diuresis will not be effective.
Can I drink alcohol while taking Loperamide
Alcohol shouldn’t be taken together with loperamide. Alcohol can increase CNS side effects of loperamide such as drowsiness, dizziness and difficulty concentrating. Some patients, especially elderly may also experience impairment in thinking and judgment.
Patients need to avoid or limit the use of alcohol while being treated with loperamide. Never use more recommended dose of loperamide, and avoid activities that require mental alertness such as driving or operating machinery until you know how the medication affects you.
Loperamide and simethichone combination
Loperamide/simethicone is a fixed combination in one medicine that is used to treat the symptoms of diarrhea accompanied with bloating, pressure, and cramps from gas that usually follow loperamide use. It is an antidiarrheal and antiflatulent combination. It works by slowing the bowel movement but it also breaks up gas bubbles to make gas easier to eliminate.
Can loperamide cause paralytic ileus?
Paralytic ileus is intestinal blockage in the absence of an actual physical obstruction. It is caused by a malfunction in the nerves and muscles in the intestine that impairs digestive movement.
Paralytic ileus was described among people who take Imodium, especially in patients who are male, 60+ old, and have been taking Imodium for < 1 month. Loperamide must be discontinued promptly when constipation, abdominal distention or ileus develop.
Can loperamide cause electrolyte loss?
Fluid and electrolyte reduction often occur in patients who have diarrhea. In such cases, appropriate fluid and electrolytes intake is very important. The use of Loperamide does not exclude the need for appropriate fluid and electrolyte therapy.
Loperamide and Quinidine interaction
Loperamide can’t pass into CNS and cause narcotic-like effects mostly because of the efflux mechanism by P-glycoprotein. However, coadministration of P-glycoprotein inhibitors such as quinidine may potentially permit loperamide to cross the blood–brain barrier and produce central narcotic-like side effects.
It has been found that combination of these two drugs can produce respiratory depression, due to central opioid actions. Common P-glycoprotein inhibitors are also: ritonavir and ketoconazole, among others.
Can I take loperamide and clarithromycin together?
Coadministration of loperamide and may enhance the gastrointestinal absorption or inhibit loperamide metabolism, because clarithromycin is potent CYP450 3A4 or 2C8 inhibitors and may increase the plasma levels and adverse effects of loperamide.
High concetrations of loperamide, including through abuse or misuse, has been related with dangerous and potentially fatal cardiac adverse effects such as syncope, arrhythmia, and cardiac arrest due to prolongation of the QT interval.
Can I take loperamide and diltiazem (Cardizem) together?
Coadministration of loperamide with drugs that may inhibit the P-glycoprotein efflux transporter may increase the concentrations of loperamide in plasma and CNS. Inhibition of P-glycoprotein in the intestine may increase loperamide systemic absorption while inhibition in the blood brain barrier enhances loperamide entry into the CNS. Opioid and other adverse effects may be facilitated.
Can I take loperamide and gemfibrozil (Lopid) together?
Coadministration of loperamide and gemfibrozil may enhance the gastrointestinal absorption or inhibit loperamide metabolism as it is potent CYP450 3A4 or 2C8 inhibitors and may increase the plasma concentrations and the risk of causing adverse effects.
Can I take loperamide and Plavix together?
Coadministration of loperamide and Plavix may enhance the gastrointestinal absorption or inhibit the metabolism of loperamide increasing the plasma concentrations and adverse effects of loperamide.
Can I take ranitidine and loperamide together?
Ranitidine may considerably increase loperamide blood levels. This can lead to very serious and potentially fatal complications such as irregular heart beat and cardiac arrest. The chances are much higher, especially if you use more than the recommended doses of loperamide.
Patients with heart condition called congenital long QT syndrome or other cardiac diseases such as conduction abnormalities or electrolyte disbalance such as magnesium or potassium loss caused by severe or prolonged diarrhea or vomiting. Patients should never exceed the dose, frequency or duration of use of loperamide as recommended on the product label or by your doctor prescription
Can I take loperamide and spironolactone together?
There is an interaction between these two drugs. Spironolaction can increase loperamide blood levels. This can lead to very serious and potentially fatal complications such as irregular heart beat and cardiac arrest. The chances are much higher, especially if you use more than the recommended doses of loperamide.
Is loperamide a controlled substance?
When it was originally approved for medical use in the US, loperamide was considered as a narcotic drug and was put into Schedule II of the Controlled Substances Act in 1970. Then it was transferred to Schedule V on 17 July 1977 and finally decontrolled on 3 November 1982.
Can I give Imodium to the dogs?
Imodium is used to treat diarrhea in humans but may be also prescribed for pets. It is also effective in conditions such as malabsorption and maldigestion in pets. In such cases pets are not extracting enough nutrients from their food. Treatment of the pet with Imodium should typically not last longer than 2 days. If your pets have diarrhea for more than 48 hours you should contact your veterinarian immediately to prevent dehydration.
If it is used in liquid form the correct dosage of Imodium may be different depending on the concentration. In that case you should seek advice from your vet if using the liquid form of Imodium. If it is used in pill form you should administer 0.05 mg per pound of pet weight, and should be given every 8 hours.
Similar to all other liquid medicines, Imodium also contains a small amount of alcohol which may be toxic to dogs, and thus it’s always better to use pills. Never exceed dosage unless instructed to do so by your vet. Treatment shouldn’t last for more than two days.
Both, generic form loperamide and Imodium are safe for use in dogs and is commonly prescribed by vets for dogs with diarrhea. However, there are some medicines which you should never mix with this drug.
Imodium and opiate withdrawal
One of the unpleasant symptoms of opiate withdrawal is diarrhea. Loperamide can be way helpful in this situation, as it works by slowing down digestion and the bowel movement preventing diarrhea and weakening the pain from the stomach cramps. Loperamide works on opiate receptors in intestines so it can be used to reduce and even stop withdrawal symptoms.
Many patients have been using Imodium for opiate withdrawal treatment for a while, but some of them credited its magnificent success to the fact that it stops diarrhea so well that they completely forget that it actually takes away the withdrawal from opiates.
Also, because Imodium is available as OTC very cheaply, patients have been turning to loperamide for opiate withdrawal for a long time, thus it becomes one of the most popular medicine used by recovering opiate addicts.
Here is a good taper schedule for administrating loperamide for opiate withdrawal:
- Day one: 40mg taken once when you wake up
- Day two: 34mg of loperamide taken in the morning
- Day three: 26mg taken during the day
- Day four: 20mg taken in the morning
- Day five: 14mg taken in the morning
- Day six: 8mg taken in the morning
- Day seven: 2mg in the morning
- Day 8 through 30: Take CalmSupport to ease the rebound withdrawals and make a smooth transition off of opiates completely.
Never take Imodium for more than 7 days.
Precautions when using loperamide for opiate withdrawal
Imodium is considered as a safe drug if it is used in recommendable doses. However, it is used in much higher doses for opiate withdrawal. In high doses, loperamide can be addictive, so keep a close eye on your intake. It is recommended that you can take Imodium or loperamide for opiate withdrawal for no longer than 3 to 4 days, and up to maximum of 7 days maximum in rare cases.
Hydration is vital when taking loperamide for opiate withdrawal, so make sure you are drinking enough water. Imodium will cause constipation so it recommendable to except fluids also increase your fiber amounts. Imodium is known to have extremely long half life, so if you take large doses of Imodium for opiate withdrawals abruptly discontinue you may experience unpleasant withdrawal symptoms.
Can I take loperamide and Pepto Bismol together?
It is not recommended to take these two drugs together. It won’t harm you if you combine them, but the pepto bismol might bind up the loperamide from Imodium and make the Imodium less effective. Finally, if it is diarrhea you want to treat, pepto bismol is not that effective. Skip the pepto bismol in that case and just use the Imodium.
Can I take Loperamide and Tylenol together?
Since there are no important interactions between these two drugs, they can be taken together safely.
Can I take Loperamide and Tums together?
Since there are no found interactions between these two drugs, their combination is considered as safe.
“Are dulcolax laxative suppositories safe during pregnancy?”
