Contents
- What is maculopapular rash?
- How maculopapular rash looks like? What are signs and symptoms?
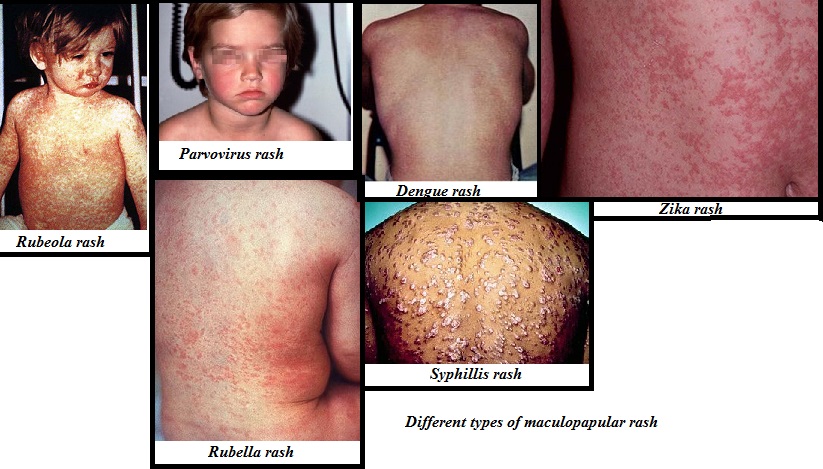
- What are the causes of maculopapular rash? Different types of maculopapular rash
- Viral/bacterial infections and maculopapular rash
- Rubeola (Measles) infection and maculopapular rash
- Rubella (German measles) infection and maculopapular rash
- Roseola (Exanthema Subitum) and maculopapular rash
- Parvovirus B19 (Erythema Infectiosum or 5th Disease) and maculopapular rash
- Chikungunya viral infection and maculopapular rash
- Dengue Fever and maculopapular rash
- Infectious mononucleosis and maculopapular rash
- Syphilis and maculopapular rash
- HIV 1 infection and maculopapular rash
- Zika virus and maculopapular rash
- Ebola virus and maculopapular rash
- Maculopapular rash caused by allergy
- Systemic and rheumatologic diseases as a cause of maculopapular rash
- Maculopapular rash after transplantations
- Niacin-induced maculopapular rash
- Sea bather’s eruption and maculopapular rash
- Arsenic intoxication and maculopapular rash
- Drug-induced maculopapular rash
- Maculopapular rash diagnosis
- Differential diagnosis for Maculopapular rash
- Maculopapular rash treatment
What is maculopapular rash?
Maculopapular rash is a skin condition belonging to the class of rash, which is characterized by red and flat area of the skin covered with small red confluent bumps. However, the red background of the skin may not me manifested in cases of dark skin. The medical term “maculopapular” describes macules which are flat, small, discolored spots on the skin surface and papules which are small, raised bumps.
It can be itchy sometimes, and it can last from 2 days to 3 weeks depending on the cause and severity. Generally when papules are not manifested, macular rashes don’t need a treatment but if it persists for longer than 2 weeks, then you should see a doctor. Underlying medical problem like measles and syphilis are common causes of this type of rash. Weaken immune system is another one.
Maculopapular rash in children is mostly caused by viral or bacterial infections. In adults, drugs and allergies are most common causes. Other medical terms for maculopapular rash may include morbilliform eruption or exanthematous eruption also known as exanthema.
How maculopapular rash looks like? What are signs and symptoms?
Because of the present skin inflammation, maculopapular rash appears to be reddened or erythematous. Macules are flat blemishes or discolorations with about 1 cm in diameter. If they exceed 1 cm they are called patches. Papules are elevated lesions measuring less than 1 cm in diameter.
In some cases papules can exceed 1 cm in diameter, and then they are called plaques which are palpable lesions elevated on skin surface or nodules which are larger and more firm papules with a significant vertical dimension. When these two are manifested together at the same time they identified maculopapular rash as a smooth skin rash or redness covered with elevated bumps.
In some cases (depending on causes) maculopapular rash can be manifested with: pustules which are described as papules containing purulent fluid, vesicles which are papules containing clear serous fluid, bullas which are larger type of vesicles (>1 cm in diameter) or urticaria described as a wheal or hive.
The papules can be warm and itchy and may change their color from red to other colors depending on the severity and nature of the disease but also on the duration of the same.
Since maculopapular rashes are mostly caused by infections and because of weaken body immune responses, more than one symptom may also appear. These may include:
- fever
- headache
- nausea
- vomiting
- breathing issues
- muscle pain
- dry skin
These symptoms may be a sign of an infection, which may be potentially contagious. Therefore only a doctor/dermatologist can provide proper diagnosis. Thus, make an appointment with your doctor if you exhibit such symptoms.
Maculopapular rash classification
There are 2 particular classifications of maculopapular rashes
By rash distribution maculopapular rash can be:
- Localized – macules and papules are concentrated in the certain part of the body or
- Generalized – rash is distributed on the most parts or at the whole body
By duration, maculopapular rash can be divided in 3 groups:
- Acute maculopapular rash that lasts less than 4 weeks
- Subacute maculopapular rash that lasts 4-8 weeks
- Chronic maculopapular rash if lasts for more than 8 weeks
What are the causes of maculopapular rash? Different types of maculopapular rash
Numerous causes may lead to maculopapular rash. In general, the most common causes are:
- Viral infections
- Bacterial infections
- Rickettsial infections
- Medicines
- Hypervitaminosis
- Allergy and hypersensitivity reactions
- Autoimmune diseases
- Systemic disorders
- Rheumatological diseases
- Weaken immune system
- Arsenic intoxications
Viral/bacterial infections and maculopapular rash
Different viral (mostly) and bacterial infections may cause maculopapular rash. Some of them are:
- EBV virus infection
- Measles
- Syphilis
- Scarlet fever
- Hand, foot, and mouth disease
- Herpes
- Hepatitis B or C infection
- Zika virus
- Ebola virus
- HIV virus
- Roseola
- Chikungunya Virus
- Dengue virus
- Parvovirus B19
- Rickettsia rickettssi (Rocky Mountain Spotted Fever)
- Cytomegalovirus (CMV)
- Enteroviruses
- Treponema pallidum (Secondary Syphilis)
- Borrelia burgdorferi (Lyme Disease)
- Rickettsia prowazekii (Louse-Borne Typhus)
- Rickettsia typhi (Murine Typhus)
- Salmonella typhi (Typhoid Fever)
- Chlamydia psittaci (Psittacosis)
- Streptobacillus moniliformis (Rate-Bite Fever)
- Spirillum minus (Rate-Bite Fever)
- Leptospira (Leptospirosis)
- Ehrlichia and Anaplasma (Ehrlichiosis)
- Filovirus
- Meningococcaemia
- Staphylococcal scalded skin syndrome (SSSS)
Rubeola (Measles) infection and maculopapular rash
Measles or Rubeola is a highly contagious viral infection caused by the measles virus (Morbilli virus). Initial signs and symptoms typically include fever, often greater than 40 °C, cough, runny nose, and inflamed eyes. A rash (telltale) is the hallmark of the disease. Koplik’s spots which are small white spots inside the mouth are typical sign of this disease and usually begin 2 or 3 days after symptoms begin.
Maculopapular rash cause by measles is the common in children. It usually starts appearing on the hairline and behind the ears spreading through the trunk and extremities typically 3-5 days after the start of symptoms.
Symptoms typically develop 10–12 days after exposure to an infected person and last about 7–10 days. If the rash becomes desquamated and brownish, then it is starting to fade away. Usually the rule is that the order on which it appeared follows the order how it fades away. The Koplik’s spots commonly disappear after the onset of rash.
Rubella (German measles) infection and maculopapular rash
Rubella, or so called German measles or three-day measles is viral infection caused by the rubella virus. A rash may start about 2 weeks after exposure and last for 3 days. Maculopapular rash caused by Rubella is spreading on the body from face downwards.
Skin rash is not as bright as in the case of Rubeola and is sometimes itchy. Swollen lymph nodes are also often and may last for a few weeks. Fever, sore throat, and fatigue, joint pain may also occur.
Roseola (Exanthema Subitum) and maculopapular rash
Roseola occurs in children who are less than 3 years old and is caused by two human herpesviruses, HHV-6 and HHV-7, which are sometimes defined to collectively as Roseolovirus. The maculopapular rash in the case of Roseola is scattered even though the face often stays unaffected. Rash usually appears after the fever disappears.
Parvovirus B19 (Erythema Infectiosum or 5th Disease) and maculopapular rash
Erythema infectiosum also called fifth disease is commonly a benign condition in children at 3-12 years of ages which is characterized by a typical slapped-cheek look and lacy exanthem. It is caused by the infection of human parvovirus (PV) B19, which is an erythrovirus. Maculopapular rash appears bright-red that makes children to look like they were slapped on the face.
This is caused by fever that occurs before the appearance of the rash. Occasionally parvovirus rash may spread over the the nose or around the mouth. Some children may also develop a red and lacy on the upper arms, torso, and legs. The maculopapular rash typically lasts a couple of days and may be itch. Rarely, it can last for several weeks. Patients are usually no longer contagious once the rash has appeared.
Chikungunya is a viral disease transmitted by mosquitoes infected by Chikungunya virus. The virus is spread between people by two mosquito’s species: Aedes albopictus and Aedes aegypti. It causes fever and severe joint pain. Maculopapular rash is also one among other manifestations. The maculopapular rash commonly appears after the itchiness and redness of the skin.
It spreads from the trunk to the face and limbs. Rash occurs in 40-50% of cases, generally two to five days after onset of symptoms. In some cases petechiae may also be noted.
Dengue Fever and maculopapular rash
Another infectious disease spread by mosquitoes is dengue. It is caused by dengue virus and is manifested with high fever, rash and joint pain. A rash occurs in 50–80% of cases with beginning symptoms called flushed skin, or later, after 4–7 as a measles-like rash. A rash is sometimes described as “islands of white in a sea of red” has also been observed.
Infectious mononucleosis and maculopapular rash
Infectious mononucleosis is an infection caused by the Epstein–Barr virus (EBV). In very rare cases rash can be manifested, usually occuring on the arms or trunk, which can be macular (morbilliform) or papular. Ampicillin and amoxicillin use are not recommended during acute Epstein–Barr virus infection since it has been shown that in many cases diffuse rash has been developed.
Syphilis and maculopapular rash
Syphilis is a sexually transmitted disease caused by the bacterium Treponema pallidum. In secondary syphilis a diffuse rash most commonly occurs, and is usually localized on the palms of the hands and soles of the feet, but it can spread throughout the body.
The maculopapular rashes can be very serious in cases with Syphilis as they may rupture and form ulcerative blisters which can be very painful. Syphillis rashes may form broad, flat, whitish, wart-like lesions known as condyloma latum on mucous membrane.
HIV 1 infection and maculopapular rash
The type 1 HIV infection usually causes maculopapular rashes. This is the reason why maculopapular rash is also known as HIV rash. In such patients maculopapular rash is present as one of the earliest signs of the virus. It is a primary form of HIV infection that occurs at different parts of the body particularly on the face, trunk, and hand palms. In the mouth and genitals, maculopapular rash poses as ulcers. It lasts about 2-3 weeks.
Zika virus and maculopapular rash
Zika, is an contagious condition caused by the Zika virus. It is manifested with fever, red eyes, headache, joint pain and a maculopapular rash. Zika disease is possibly best-known due to its possibility to pass from mother to child during pregnancy causing microcephaly and other brain defects in newborns.
Zika rash can be red and raised and often itchy and uncomfortable. The rash often begins on the face and spreads. Zika rash will disappear once the virus is healed, so there should be no worries about long-term effects.
Ebola virus and maculopapular rash
Ebola is a viral hemorrhagic fever caused by ebolaviruses. In about 50% of cases cases, maculopapular rash may be developed on the skin manifested as a flat red area covered with small bumps, usually 5-7 days after symptoms begin.
Maculopapular rash caused by allergy
A maculopapular type of rash that begins immediately after exposure to allergens (allergies to food and insect bite or sting) may be also caused. This typically happens after minutes to few hours after exposure to the allergen. In some cases a maculopapular rash may break out before hives do. A person with maculopaular rash caused by allergy may also experience increased heart rate and breathing problems.
Systemic and rheumatologic diseases as a cause of maculopapular rash
Different systemic or rheumatologic diseases may lead to maculopapular rash. Most common causes are:
- Acute graft-versus-host disease (stem cell or bone marrow transplant)
- Kawasaki disease (mucocutaneous lymph node syndrome) and
- Still’s disease (juvenile rheumatoid arthritis)
Maculopapular rash after transplantations
Maculopapular rash has been also described as a condition known as graft-versus-host disease (GVHD) that can be developed after hematopoietic stem cell transplantation (bone marrow transplant) which can be seen within 1 week or several weeks after the transplantation. In the case of GVHD, the maculopapular rash may progress into a several condition similar to toxic epidermal necrolysis.
Niacin-induced maculopapular rash
This type of maculopapular rash can be induced as a result of intaken large doses of niacin or no-flush niacin of 2000 – 2500 mg used for the management of low HDL cholesterol.
Sea bather’s eruption and maculopapular rash
Maculopapular rash may be also a symptom of a condition known as Sea bather’s eruption that most usually affects swimmers in some Atlantic locales including: Florida, Caribbean, and Long Island. It is provoked due to hypersensitivity to stings from the larvae of the sea anemone Edwardsiella lineate or the thimble jellyfish Linuche unguiculata. The rash appears where the bathing suit contacts the ski and is usually stinging and pruritic.
Arsenic intoxication and maculopapular rash
This type of rash can also be caused due to acute arsenic poisoning, appearing 2 weeks after exposition.
Drug-induced maculopapular rash
Drugs such as antibiotics, anticonvulsants, allopurinol may induce maculopapular rash as one of their adverse reactions. One study reviewed 50,000 patients with drug skin eruptions and in 91% cases drug eruptions presented as maculopapular rash. Increased risk was observed with factors such as immunosuppression, in elderly and female gender.
Maculopapular rash is categorized as a type IV or delayed cell-mediated reaction that is caused by body’s hypersensitivity of a drug or its metabolite.
For maculopapular rash it is suspected to be induced after new drug administration within 4-12 days. It may be confirmed after drug discontinuation as it will disappear after some time. It will reappear once the medicine that cause adverse reaction is readministered.
Penicillin (amoxicillin, ampicillin) induced maculopapular rash
Most antibiotics are known to cause rash as a side effect. However, it looks like that penicillin antibiotics such as ampicillin and especially amoxicillin causes a rash more often than others. Penicillin occurs to be most common drugs that a lot of patients are sensitive to. About 10 % of people report allergic reactions to penicillin. It is expected that incidence is much higher.
Amoxicillin is known to cause 2 types of allergic skin manifestations: Hives and Maculopapular rash. Hives are raised, itchy, white or red bumps on the skin that appear after 1-2 doses of the drug, they may be allergic to penicillin. On the other hand, smaller and paler patches commonly accompanied with the red patches on the skin are the signs of amoxicillin induced maculopapular rash.
It often develops among 3-10 days after beginning the therapy with amoxicillin. Girls are usually more sensitive than boys in a developing a rash after taking amoxicillin. Also, children who have mononucleosis and then take antibiotics may be more likely to get the rash.
While hives are most usually caused by allergies, it can’t be concluded for sure what causes maculopapular rash to develop. If your child gets a maculopapular rash without signs of hives or other symptoms, it doesn’t necessarily be that they are allergic to amoxicillin. They are simply more sensitive to amoxicillin without having a true allergy.
If you notice your child get allergic reaction after taking amoxicillin, you should call your doctor immediately, as the allergic reaction could get worsen. Never give another dose to your of this medication without talking to you doctor firs. Call emergency if your child is having difficulty breathing or shows signs of swelling after amoxicillin or any other drug use.
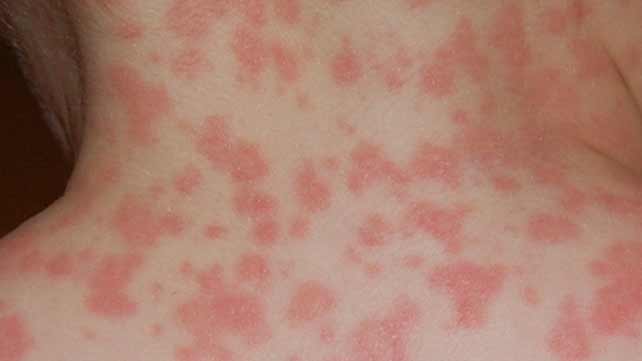
Anticonvulsant drug (barbiturates, carbamazepine) induced maculopapular rash
Different anticonvulsant (antiepileptic) drugs including carbamazepine, phenytoin, fosphenytoin, phenobarbital, lamotrigine and valproic acid may cause skin rashes as side effects. Some racial groups have been shown to be especially prone to cutaneous side effects after anticonvulsants use.
For example Han Chinese and different South-east Asians populations who have a particular HLA-B allele are considerably more likely to develop severe allergic skin reactions such as Stevens Johnson syndrome or toxic epidermal necrolysis after anticonvulsants use. Laboratory genetic testing for the particular genes before anticonvulsant use may be useful in identifying patients at risk.
Allopurinol (Zyloprim, Aloprim) induced maculopapular rash
Allopurinol (Zyloprim, Aloprim) is drug used to prevent attacks of gout and kidney stones and also treats different complications of cancer chemotherapy. Allopurinol rashes can vary from a mild skin irritation to a severe allergic reaction. Milder form of rashes may be manifested with: redness, itching or small bumps on a small surface of the body.
Severe rashes may produce a wide-spread skin rash characterized with peeling, hives, fever and joint pains. If you develop a skin rash during allopurinol treatment you should stop taking the drug immediately and then go and see your physician.
Maculopapular rash diagnosis
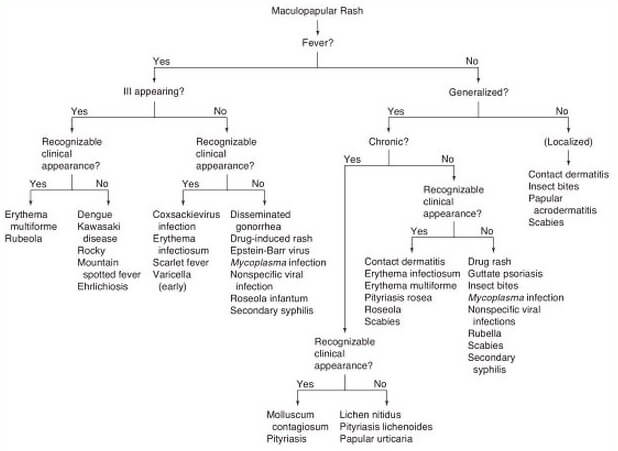
Following guideline diagnostic diagram may be helpful to determine the real cause of maculopapular rash. It also guides health professionals how to proceed and what to do in order to give the patient appropriate treatment.
If maculopapular rash is present, the first and most important question is to answer whether patient has a fever or not. If the answer is yes, it should be determined if the patient is ill or not. In that case patient possibly has erythema multiforme, Kawasaki disease, rubeola, dengue, Rocky Mountain spotted fever or ehrlichiosis.
If the patient doesn’t appear ill, then Coxsackie virus, scarlet fever, erythema infectiosum, gonorrhoea, varicella, drug-induced rash, Epstein-Barr virus, Roseola infantum, Mycoplasma infection, secondary syphilis, or viral infection should be considred
If the patient does not have a fever, it should be determined if the rash is localized or generalized. If it is localized on the exact part of the body, the maculopapular rash may be caused by contact dermatitis, scabies, insect bite or papular acrodermatitis. If generalized, it should be considered if it is acute or chronic. If it is chronic, the patient may have: pityriasis, molluscum contagiosum, pityriasis lichenoides, lichen nitidus or papular urticaria.
If it is acute, the patient may have erythema infectiosum, contact dermatitis, erythema multiforme, pityriasis rosea, scabies, roseola, drug-induced rash, guttate psoriasis, insect bite, rubella, Mycoplasma infection, secondary syphilis, or other viral infections.
Except physical examination, laboratory tests such as: complete blood count test, culture test of pustules, syphilis tests and cerebrospinal fluid tests should be performed. In general, examination of the lung, ENT, genitals, joints and nerves should be also conducted.
Differential diagnosis for Maculopapular rash
Maculopapular rash may be mistakenly called macule, papule, patch, nodule, plaque, vesicle, or pustule. Confusion and intense headache may indicate gonococcemia. Inflammation of the joints indicates meningococcemia. Breathing problems may be related pharyngitis or anaphylaxis. Purulent urethral drainage may also be linked with maculopapular rash on private parts of the body.
Maculopapular rash treatment
The proper management of maculopapular rash depends on the disease, the severity of the disease and also the age of the patient. There are number different methods that can be used for symptomatic relief of maculopapular rash.
Intravenous fluids and oral rehydration for maculopapular rash
Mild cases of Dengue fever should be treated with intravenous fluids and oral rehydration. However, severe cases require blood transfusions. Pateients infected with the Epstein-Barr Virus are also suggested to take rest and as well as increase their fluid intake.
Painkillers for maculopapular rash
Painkillers such as NSAIDs (ibuprofen, diclofenac, naproxen, etc) can be used for pain prelief associated with rash especially in the case of EBV (Epstein-Barr Virus) as the cause of the maculopapular rash.
Chloroquine for maculopapular rash
In the case of Chikungunya virus induced maculopapular rash and positive serologic tests to this virus, chloroquine can be prescribed. This anti-inflammatory which helps palliates the disease and its symptoms.
Ultraviolet and Gamma Radiations
These 2 radiations-type treatments may be the last resort for most severe cases of Marburg hemorrhagic fever caused maculopapular rash.
“What is the uvula and its function? How does your uvula get swollen?“