Contents
- What is phencyclidine?
- How does phencyclidine look like?
- Phencyclidine history of use
- Phenyciclidine trend of use
- What is “FRY“?
- Ketamine vs. phencyclidine
- How is phencyclidine most commonly abused?
- Whar are street names for phencyclidine?
- Phencyclidine mechanism of action
- Phencyclidine recreational use
- What happens with PCP in the body?
- Neurophysiology of phencyclidine
- Phencyclidine effects on behaviour and performance
- Is phencyclidine a controlled drug?
- Pharmacokinetics of phencyclidine and routes of use
- Phencyclidine discriminative stimulus effects
- Phencyclidine tolerance
- Phencyclidine reinforcing effects
- Phencyclidine toxicity
- Phencyclidine drug testing
- Phenyciclidine withdrawal
- Is PCP Addictive?
- Phenyciclidine treatment
- PCP urine, blood and hair testing
What is phencyclidine?
Phencyclidine is a generic name for a hallucinogenic drug formerly used as a veterinary anesthetic, and briefly as a general anesthetic for humans. Strucutrally, it is similar to ketamine and in many of its effects. Like ketamine, it can produce a dissociative state. It exerts its pharmacological action through inhibition of NMDA receptors. As a drug of abuse, it is known as PCP and Angel Dust.
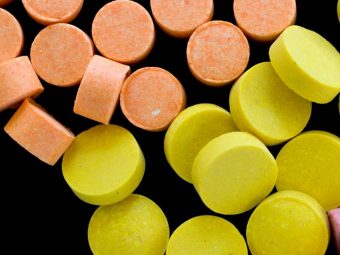
How does phencyclidine look like?
Phencyclidine is a bitter-tasting, white crystalline powder that is easy to dissolve in water or alcohol. Phencyclidine may be dyed various colors and often is sold as a tablet, capsule, liquid, or powder.
Phencyclidine history of use
Although PCP and drugs of similar chemical structure (arylcyclohexylamines) are often called hallucinogens, they rarely produce hallucinations, and the sensory distortions or apparent hallucinations that are produced are not the same type as LSD-induced hallucinations. Instead, phencyclidine belongs to a unique class of drugs called the dissociative anesthetics.
Phencyclidine was developed in the 1950s as an anesthetic for veterinary medicine and later was tested in human surgical patients. There was great potential for PCP as an anesthetic because it produced minimal effects on the heart and breathing was not suppressed.
Unfortunately, the adverse side effects of PCP (e.g., dysphoria and psychotic symptoms) led to a termination of the human clinical trials. The drug is no longer manufactured for veterinary use because supplies were diverted(stolen) and the drug became widely abused in the 1970s.
Phenyciclidine trend of use
Patterns of PCP use are similar to LSD. Most use is experimental or occasional, but unlike LSD, some occasional users become heavy chronic users. Unfortunately, even though tolerance does develop to the reinforcing effects of dissociative anesthetics, the tolerance is not severe enough to discourage continuous use as is the case with LSD.
Not until the decline of LSD in the 1970s did PCP use start to increase. Before PCP became popular in its own right, it was more widely used than most people suspected because it was often mixed with other drugs or sold as something different. While its use has declined, it is still popular in some metropolitan areas and among certain groups who continue to take it by itself or mixed with marijuana or cocaine.
The small percentage of users has continued to decrease. In 2004 and 2008, roughly 0.5% of high school students in the United States reported using PCP within the past 30 days. In the United Kingdom and Canada, the trend has been fairly stable at low percentages over the last few years.
What is “FRY“?
Fry is a street term for marijuana or tobacco cigarettes that are dipped in PCP (phencyclidine) and/or embalming fluid, and then dried.
Embalming fluid is a compound of formaldehyde, methanol, ethanol (ethyl alcohol), and other solvents. Embalming fluid reportedly produces a hallucinogenic effect and causes the cigarette to burn more slowly, potentially resulting in a prolonged high.
Ketamine vs. phencyclidine
Ketamine, a drug chemically similar to PCP, is now used as a veterinary anesthetic and, in special cases, for anesthesia in humans. This drug is less powerful and shorter acting than PCP.
How is phencyclidine most commonly abused?
Phencyclidine abuse, mainly in pill form, peaked in the late 1970s and markedly declined throughout the 1980s and early 1990s. The most common route of administration in use in the 1990s was smoking. Phencyclidine is often added to marijuana cigarettes, and it is commonly used while people are also drinking alcoholic beverages.
Whar are street names for phencyclidine?
Street names for PCP are ‘‘angel dust’’ or ‘‘crystal’’; it is called ‘‘space base’’ when combined with cocaine.
Phencyclidine mechanism of action
Phencyclidine acts as an antagonist at the N-methyl-D-aspartate (NMDA) receptor-channel complex, which is one type of excitatory amino acid receptor that is selectively activated by the agonists NMDA and glutamate. By definition, agonists produce stimulation while antagonists block the effects of agonists.
When either glutamate or NMDA bind to the receptor, a channel within the cell membrane opens to allow sodium, calcium, and potassium ions to flow into and out of the cell. This movement of ions across the cell membrane causes a depolarization of the membrane which, if sufficiently large, causes the cell to fire.
When the cell fires, an electrical charge passes along its membrane and neurotransmitter (chemicals that allow cells to communicate with each other) are released. Thus, glutamate and NMDA are important for normal cell-to-cell communication within the body. PCP, as well as TCP, ketamine and dizocilpine is representative of compounds that act as noncompetitive antagonists at the NMDA-receptor complex.
The binding site for PCP resides within the channel and binding to this site physically prevents calcium and sodium ions from entering the cell while at the same time preventing potassium ions from leaving the cell. Blocking the movement of ions through the cell membrane in turn prevents the neuron from firing.
By simply occupying the receptor without activating it, competitive antagonists prevent NMDA from binding to and activating the receptor. Unlike noncompetitive antagonists, competitive NMDA-antagonist effects can be surmounted by higher doses of the agonist. However, the end result of both noncompetitive and competitive antagonists is a reduction of neuronal firing.
Phencyclidine recreational use
PCP started to emerge as a recreational drug in mostcities in the United States in 1967. In 1978, People magazine and Mike Wallace of 60 Minutes called PCP the country’s “number one” drug problem. Though recreational use of the PCP had always been relatively low, it started declining significantly in the 1980s. According to the studies, the number of high school students admitting to trying PCP at least once fell from 13% in 1979 to less than 3% in 1990.
What happens with PCP in the body?
PCP is weak, lipid-soluble bases and can be inhaled, injected, or taken orally. A moderate dose of PCP is 5 to 10 mg. The effects of PCP are felt within a minute of inhalation or intravenous injection and from 20 to 40 minutes after oral administration. Peak effects usually occur between 10 and 90 minutes, and the effects may last from 4 to 8 hours. Drug levels fall rapidly at first as the drug is absorbed into body fat; however, low levels may persist in the body for several weeks as the drug is released from body fat.
Neurophysiology of phencyclidine
The dissociative anesthetics appear to alter the functioning of norepinephrine, dopamine, acetylcholine, and serotonin, but it is believed that the principal effect responsible for their reinforcing properties is that they block NMDA receptors for glutamate and aspartate, which are excitatory transmitters in many parts of the brain, including the cortex.
PCP and ketamine have a binding site embedded in the ion channels normally activated by NMDA receptors. When the binding site is occupied by PCP, the NMDA receptor ion channel is blocked, making these transmitters ineffective.
This mechanism is thought to be similar to that of the alcohol molecule. PCP appear to act as reinforcer by influencing glutamate activity, and thereby dopamine release, in the mesolimbic and mesocortical pathways in a manner similar to the barbiturates and benzodiazepines.
Phencyclidine effects on behaviour and performance
The dissociative anesthetics are known to cause amnesia for events that occur while under the influence of the drug. Although no studies of the effects of PCP on memory in humans have been conducted, PCP does seem to be more disruptive of memory in nonhumans than LSD, THC, opioids, and other psychoactive drugs.
It is known that NMDA receptors are vital in the formation of long-term memories, and so it is not surprising that NMDA antagonists like PCP and ketamine are powerful amnesic drugs. In addition, it has been demonstrated that PCP may induce a type of thought disorder very similar to that seen in schizophrenic patients. PCP is not hallucinogenic in the same sense as LSD.
Taken at usual doses, the dissociative anesthetics cause relaxation, warmth, a tingling feeling, and a sense of numbness. There are euphoric feelings, distortions in body image, and a feeling of floating in space. When these effects wear off, they are sometimes followed by a mild depression that may last from 24 hours to a week. At higher doses, the user may become stuporous or even comatose.
Psychotic behavior occurs frequently and may include anything from manic excitation to catatonia, in which the user assumes one position and does not move for a prolonged period of time. There may be sudden mood changes accompanied by laughing and crying; disoriented, confused, and delusional thought; drooling; and repetitive (stereotyped) actions. This psychotic state often disappears as drug levels decline, but sometimes the psychosis requires hospitalization and lasts for weeks.
Is phencyclidine a controlled drug?
PCP is a Schedule II substance in the United States and its ACSCN is 7471. Its manufacturing quota for 2014 was 19 grams.
It is a Schedule I drug by the Controlled Drugs and Substances act in Canada, a List I drug of the Opium Law in the Netherlands, and a Class A substance in the United Kingdom
Pharmacokinetics of phencyclidine and routes of use
PCP use in humans occurs through several routes of administration, including intranasal (snorted), intravenous, oral, and inhalation (smoked). When PCP is smoked in parsley cigarettes, approximately 70 percent of the total amount of PCP is inhaled. Of this amount, 38 percent is inhaled as PCP and 30 percent is inhaled as phenylcyclohexene, a by-product of PCP created when it is heated.
Peak blood concentration of PCP occurs after only five to ten minutes, which is occasionally followed by a second peak one to three hours later. PCP is predominantly excreted in urine after intranasal, intravenous, and oral administration. The rate of PCP elimination through the kidneys depends on both urine pH and urine-flow rate. More specifically, PCP elimination occurs more rapidly when urine is acidic and when urine is passed rapidly.
Phencyclidine discriminative stimulus effects
One useful method of evaluating the pharmacological characteristics of PCP, as well as a variety of other drugs, is the drug-discrimination procedure. Typically, animals that are slightly food restricted are trained to respond for food on one lever after drug administration and on another lever after saline.
On days when the drug is administered before the session, responding on the drug-associated lever results in food delivery while responding on the saline-associated lever does not. Conversely, on days when saline is administered before the session, responding on the saline-associated lever results in food delivery while responding on the drug-associated lever does not.
After a number of training days, animals learn to reliably respond on the drug lever after the drug injection and on the saline lever after saline injection. Once this discrimination has been established, a number of test drugs can be administered to determine whether or not they produce effects similar to the training drug.
Test drugs that substitute for the training drug (i.e., cause responses on the drug-associated lever) are assumed to have discriminative stimulus effects that are similar to the training drug. Using this procedure, several investigators have shown that PCP and other noncompetitive antagonists produce similar discriminative stimulus effects in a number of different species.
These results suggest that the mechanisms of action of PCP and other noncompetitive antagonists, such as ketamine and dizocilpine, are similar. Furthermore, the discriminative stimulus effects of competitive antagonists such as CGS 19755, NPC 12626 and CPP were also similar to each other, which is again consistent with the notion that the mechanisms of action of competitive antagonists are similar.
Given that competitive and noncompetitive antagonists both reduce neuronal firing, it was of interest to compare the discriminative stimulus effects of these two types of antagonists. In most species, the discriminative stimulus effects of competitive and noncompetitive antagonists are very different from each other.
Another difference between the competitive and noncompetitive antagonists lies in their abilities to antagonize the discriminative stimulus effects of NMDA. While both types of antagonist are effective in blocking the convulsant and lethal effects of NMDA, competitive antagonists in general are much more effective than noncompetitive antagonists in blocking the discriminative stimulus effects of NMDA.
The noncompetitive antagonists partially antagonize NMDA but only at doses that produced substantial behavioral suppression. While most effects of NMDA are antagonized by both competitive and noncompetitive antagonists, the behavioral-suppressing effects of noncompetitive antagonists often interfere with their ability to antagonize the discriminative stimulus effects of NMDA.
Phencyclidine tolerance
Tolerance to a drug occurs when increasingly higher doses are needed to produce a specific effect or if drug effects diminish after repeated administration of the same dose of drug. It has not been possible to study tolerance to PCP in human subjects, but when interviewed, PCP users report that they increase the amount of PCP that they take over time.
Another indicator of tolerance development is that burn patients treated with ketamine for pain often require higher doses over time. It is easier to study tolerance to ketamine, PCP, and similar drugs in animals. Laboratory studies with rats have shown that tolerance developed to the effects of PCP on food-reinforced responding, to the effects of PCP and dizocilpineon steroid hormone (adrenocorticotropin and corticosterone) release, and to the cataleptic effects of ketamine.
Supersensitivity, the opposite of tolerance, occurs when repeated drug exposure produces a greater effect at a given dose. Some investigators have found that tolerance develops to some effects of PCP, such as head weaving, turning, and back pedaling, while supersensitivity occurs with other behaviors, such as sniffing, rearing, and ambulation.
Although some scientists have hypothesized that PCP tolerance and supersensitivity are mediated through non-NMDA-receptor systems, others have suggested that PCP tolerance may be mediated through the NMDA receptor system. Repeated administration of dizocilpine, a PCP-like compound, produced a reduction in the number of NMDA receptors in the rat brain, and that was correlated with tolerance to some of the behavioral effects produced by dizocilpine.
Further studies will clarify the role of different receptor systems in the development of tolerance to the effects of PCP and related compounds. Studies indicate that there are interactions between PCP and other drugs with respect to tolerance and supersensitivity of drug effects.
For example, dizocilpine blocked the development of tolerance to morphine’s analgesic (painkilling) effects, but it did not alter the analgesic effects when morphine was administered acutely. Also, dizocilpine attenuated the development of tolerance to ethanol, and it inhibited sensitization to amphetamine and cocaine.
Phencyclidine reinforcing effects
The reinforcing effects of a drug are determined by demonstrating that self-administration of the drug plus the solution it is dissolved in (vehicle) occurs in excess of self-administration of the vehicle alone. When drug-reinforced behaviour is readily achieved in the animal laboratory, it is usually a good predictor that the drug has considerable abuse liability in the human population.
The reinforcing effects of PCP have been studied using two animal models of self-administration, oral and intravenous. The intravenous route of self-administration requires the animal to make a specified number of responses on a lever or other manipulandum within a predefined time—then a fixed dose of the drug is delivered by an infusion pump via a catheter that is surgically implanted in a large vein that leads to the heart.
Studies from various laboratories have demonstrated that intravenously delivered PCP functions as a reinforcer for rats, dogs, monkeys, and baboons. Drugs that are chemically similar to PCP are also self-administered intravenously.
Theseinclude drugs that have similar receptor-binding sites in the brain, such as ketamine, dexoxadrol, and cyclazocine; and phencyclidinelike drugs that function as noncompetitive antagonists at the NMDA receptor, such as dizocilpine. Phencyclidine self-administration is more reliably obtained when the animal has a history of self-administration of a drug with similar pharmacological or discriminative-stimulus effects.
It has also been found that drugs that share discriminative-stimulus effect with PCP, such as ketamine, PCE, TCP, and ethanol, are readily substituted for PCP in self-administration studies. Oral PCP self-administration is established by presenting gradually increasing concentrations of PCP after the animal is given its daily food ration.
After sufficient quantities of PCP are consumed, food is given after the drug self-administration session, and PCP consumption usually persists. This procedure provides a long-term stable baseline to examine variables that affect PCP-reinforced behavior.
For example, alternative nondrug reinforcers, such as saccharin, reduce PCP-reinforced responding up to 90 percent of baseline if the FR for PCP is high or if the PCP concentration is very low. Free access to food decreases PCP self-administration, while even small reductions in the daily food allotment markedly increase PCP self-administration. Concurrent availability of ethanol also reduces PCP-reinforced responding.
Phencyclidine toxicity
Common physical examination findings include the following:
- Nystagmus (horizontal, vertical, or rotary) – Rotary often considered a hallmark of PCP intoxication (57-89%)
- Hypertension (57%)
- Acute brain syndrome involving confusion, amnesia, disorientation, and violence (37%)
- Agitation and violent behavior (35%)
- Tachycardia (30%)
- Bizarre behavior including public nudity (29%)
- Hallucinations and delusions (19%)
- Miosis – Often reported with a blank stare
Rare findings, usually only seen with high doses, include the following:
- Seizures (3.1%)
- Dystonia
- Ataxia
- Apnea (often seen with co-ingestants)
- Catatonia
- Coma – PCP coma usually presents with nystagmus and the absence of respiratory depression. Unlike opioid-induced coma, it does not improve with naloxone.
- Hypertensive crisis
- Myocardial infarction(non-Q wave, cardiac enzyme leak)
- Intracranial and subarachnoid hemorrhage
Other manifestations include the following:
- Hyperthermia, hyperreflexia, and muscle rigidity have been reported.
- Rhabdomyolysis with or without acute renal failure may also occur.
Is Phenyciclidine harmful?
PCP has an unfounded reputation for causing violence and uncontrollable behavior. An examination of the literature on the drug has not found any systematic evidence that this drug specifically cause violent or criminal behavior.
It is true, however, that the psychotic state induced by large doses of dissociative anesthetics causes disorientation, agitation, and hyperactivity, and that these effects have the potential for injury to the individual and others nearby. However, PCP does not seem to turn normal, innocent people into dangerous and violent criminals. Laboratory research even suggests that PCP may have a taming effect on normally aggressive animals.
As with many other drugs of abuse, it appears that chronic ketamine use is associated with long-term neurological changes. Long-lasting psychotic behavior has been reported after PCP use, even in individuals without any psychotic tendencies. This PCP psychosis may last several months in some individuals and is indistinguishable from schizophrenia as it includes both positive and negative symptoms.
Acute behavioral effects of PCP and ketamine can sometimes be responsible for injury and death. For example, because the drugs are anesthetics, rather severe injuries have been tolerated or self-inflicted without pain or any effort at avoidance.
Although the exact frequency of this sort of event has not been documented, it is probably more likely to happen with PCP than with LSD and the other serotonin-like and norepinephrine-like hallucinogens.
PCP has been shown to slow the growth of the fetus, precipitate labor, and cause fetal distress. Children born to mothers who use PCP often show muscle stiffness, tremor, irritability, and impaired attention and behavior control that may last for several years, although it is difficult to be sure that these effects are due specifically to PCP since other maternal drug use is common.
Also, usage of PCP and ketamine has been linked to widespread cell death in the developing rat brain. Blockage of NMDA receptors by PCP or ketamine for even a few hours during prenatal development appears to induce significant neurodegeneration.
Phencyclidine drug testing
- Phencyclidine can be confirmed in the body by qualitative urine toxicology screening. Serum screening for Phencyclidine is not useful clinically because the test is not readily available. Moreover, quantitative serum PCP level does not correlate with the symptoms. A fingerstick glucose test should be performed in all patients with altered mental status, as hypoglycemia can cause symptoms consistent with PCP intoxication. In addition, McCarron et al found that 20% of patients with acute PCP intoxication were hypoglycemic on presentation.
- No laboratory tests are specific for Phencyclidine intoxication, but, in addition to hypoglycemia, elevations in WBC count and BUN and creatinine levels may be seen. Serum creatine phosphokinase and urine myoglobin levels should also be measured to rule out rhabdomyolysis, especially in the patients with severe agitation.
- Consider an arterial blood gas (ABG)measurement to assess for hypoxemia and metabolic acidosis in unresponsive patients.
- Urine pregnancy tests are indicated for female patients of childbearing age.
- Do not rely on the urine toxicology screen to diagnose acute PCP intoxication.
- Chronic PCP users can have positive test results for weeks after their last use. In addition, false-positive results for PCP have also been reported with many agents, including diphenhydramine (Benadryl) and dextromethorphan, agents in over-the-counter allergy and cough formulations that can produce clinical effects similar to PCP when taken in high doses. Other reported confounders include methadone, ibuprofen, chlorpromazine, and venlafaxine. Consult the laboratory for a list of confounders. If contaminants are a concern, a gas chromatography–mass spectroscopy (GC-MS) confirmatory test can be ordered.
Phenyciclidine withdrawal
Withdrawal research with nonhumans has shown that there may be some withdrawal after continual use of PCP. The symptoms include vocalizations, grinding of the teeth, diarrhea, difficulty staying awake, anxiety, confusion, and tremors. No systematic studies of PCP withdrawal in humans have been done.
Is PCP Addictive?
PCP is considered a drug with a number of unusual effects, including hallucination and dissociation. Consequences of such effects can include:
- Fearful out-of-body experiences.
- Feelings of invincibility.
- Perceived power over others.
- Paranoia
- Violence
Repeated use of PCP, even recreationally, can have severe psychological impact. Aside from the typical dissociative effects, PCP can cause even more alarming effects. According to the National Drug Intelligence Center, users of PCP can become violent, suicidal, and experience symptoms of psychosis similar to those diagnosed with schizophrenia–such as delusions and paranoid thinking.
While withdrawal symptoms for PCP have not been established in humans, the “high” that the drug provides can help to cultivate the compulsion to use over and over–even when PCP has negatively impacted the user’s life. The official substance abuse diagnosis in cases such as these would be termed phencyclidine use disorder.
People under the active influence of PCP use may exhibit some of the mental and behavioral signs and symptoms listed above, and may act out in an extremely aggressive or violent manner. They may also appear to be very disoriented, delirious or “out of it.” Other signs to look out for include:
- Irritability
- Suspicious attitude
- Anxiety
- Depression
- Reacting to delusions
- Grandiosity
- Euphoria
- Hypersensitivity to sound
- Memory loss
- Suicidal ideation.
Phenyciclidine treatment
Management of PCP intoxication in the ED includes the following:
- After stabilizing the ABCs, treatment of PCP intoxication starts with initial supportive measures (IV, O 2, cardiac monitor). ECG may be needed to evaluate for dysrhythmias.
- Obtain a fingerstick to rule out hypoglycemia.
- Place patients in a dark, quiet room under continuous observation to minimize environmental stimuli.
- Activated charcoal for oral ingestions and co-ingestions should be considered. Multiple doses of charcoal may be beneficial in the case of large overdose. Only one dose of sorbitol should be given, usually with the initial dose. Clinicians should be aware that inappropriate administration of activated charcoal can convert relatively benign exposure (eg, mild PCP intoxication) into a very serious condition.
- Extreme violent psychotic behavior requires sedation with parenteral benzodiazepines. Seizures should be treated with benzodiazepines.
- Haldol (haloperidol) should be reserved for patients with mild, predominately psychotic symptoms, with normal vital signs.
- Butyrophenones (haloperidol, droperidol) and phenothiazines (eg, chlorpromazine) should be avoided in moderate and severe intoxications because they can lower seizure threshold, cause dystonic reactions, induce hypotension, and worsen anticholinergic symptoms, including hyperthermia.
- Hyperthermia may be treated by conventional cooling methods.
- Rhabdomyolysis is treated with intravenous hydration, urine alkalinization, and osmotic/diuretic agents. Possible caveat: There is a theoretical, but clinically unproven, concept of increased PCP reabsorption secondary to the urine alkalinization.
- For hypertensive emergencies, try to control agitation first with parenteral benzodiazepines. For persistent hypertension, intravenous nitroprusside is the agent of choice. Because of the theoretical concept of unopposed alpha effect (worsening of hypertension) and the availability of other antihypertensive agents (eg, calcium-channel blockers, intravenous nitroglycerin), pure beta-blockade should be avoided. Even labetalol, which has both alpha- (weak) and beta-blocking abilities, can be given only after alpha-blockade with phentolamine is achieved.
Acute PCP toxicity can usually be managed conservatively with an observation period of a few hours. More serious ingestions may require admission to an intensive care unit for days to weeks.
PCP urine, blood and hair testing
Urine Testing
10% of PCP is excreted unchanged in the urine. The remainder is metabolized into hydroxylate or glucuronide. Standard urine screening and gc/ms test for both PCP and its metabolites. PCP is stored by the body in fatty lipid tissue for up to several weeks. Chronic users and individuals with high body fat count are at the greatest risk of long-term detection.
Hair Testing
PCP is detectable with hair tests and is included in the standard set of substances tested for by many companies. Hair tests generally take the most recent 1.5 inches of growth and use those for testing. That provides a detection period of approximately 90 days. If an individual’s hair is shorter than 1.5 inches, this detection period will be shorter.
Blood Testing
PCP is detectable in the blood for approximately 1-3 days after use.
“What is fenethylline? What are the long term effects of fenethylline abuse?“


