Contents
- What is Amoxicillin?
- How Amoxicillin works in the body?
- Amoxicillin and Alcohol interaction? What happens if taken together?
- How long does Amoxicillin last in the body
- How long does Alcohol last in the body?
- Taking Amoxicillin 500 mg with beer
- What is “Disulfiram-like Reaction”? Can Amoxicilin cause this reaction?
- Which drugs can cause “Disulfiram-like Reaction”?
- Factors that may increase the risk of Alcohol and Antibiotic interaction
What is Amoxicillin?
Amoxicillin is a Generic name for penicillin antibiotic drug that fights bacteria.
Amoxicillin is used for the treatment of different types of infection such as: bronchitis, tonsillitis, gonorrhea, pneumonia, and infections of the nose, throat, ear, skin, or urinary tract.
It is usually used together with another antibiotic called clarithromycin for the treatment of stomach ulcers caused by Helicobacter pylori infection. This combination is sometimes used with a stomach acid reducer called lansoprazole.
This broad-spectrum semisynthetic antibiotic which is very similar to ampicillin exhibit higher serum levels after oral administration due to its higher resistance to gastric acid.
Amoxicillin is commonly prescribed together with a beta lactamase inhibitor called clavulanic acid as it is susceptible to beta-lacatamase degradation.
This combination can increase the range of action against Gram-negative bacteria, and to overcome bacterial antibiotic resistance which is mediated through β-lactamase production. The incidence of β-lactamase-producing resistant organisms, including E. coli, appears to be increasing.
Other Brand names for Amoxicilin on the market are: Moxatag, Trimox, Amoxil, Amoxil Pediatric Drops, Amoxicot, Moxilin, Wymox, Biomox, and Dispermox.
How Amoxicillin works in the body?
Amoxicillin works by binding to certain protein called penicillin-binding protein 1A or PBP-1A which is located inside the cell wall of bacteria. Amoxicillin acylate C-terminal domain of the penicillin-sensitive transpeptidase enzyme by opening the lactam ring.
Inactivation of this enzyme inhibits the third and last stage of bacterial cell wall synthesis by preventing the formation of a cross-link of two linear peptidoglycan strands.
After that, autolytic enzymes called autolysins mediate the lysis of bacteria cell. Some studies also showed that amoxicillin can interfere with an autolysin inhibitor.
Amoxicillin and Alcohol interaction? What happens if taken together?
Alcohol may alter the intensity of the pharmacological effect of Amoxicillin, so the overall actions of the combination of alcohol and Amoxicillin can be additive. Acute presence of alcohol in blood may inhibit the metabolism of Amoxicillin by saturating the liver enzyme cytochrome P450.
Half-life of Amoxicillin in blood will be prolonged, and the incidence of Amoxicillin side effects will be increased. The most common side effects that amoxicillin and alcohol may cause are: stomach upset, drowsiness and dizziness.

The table below shows the incidence of side effects after Amoxicillin administration in recommendable doses. The incidence can be increased if Amoxicillin is taken together with alcohol.
| Frequency not defined | AST/ALT elevation, Mucocutaneous candidiasis, Anaphylaxis, Diarrhea, Headache, Nausea, Vomiting, Anemia, Pseudomembranous colitis, Serum sickness-like reactions, Rash |
| Postmarketing Reports | black hairy tongue and hemorrhagic/pseudomembranous colitis, Mucocutaneous candidiasis, serum sickness–like reactions, anaphylaxis, erythematous maculopapular rashes, exfoliative dermatitis, erythema multiforme, Stevens-Johnson syndrome, hypersensitivity vasculitis, urticarial, toxic epidermal necrolysis, acute generalized exanthematous pustulosis, hepatic cholestasis cholestatic jaundice, acute cytolytic hepatitis, crystalluria, reversible hyperactivity, agitation, confusion, convulsions, anxiety, insomnia, behavioral changes, Tooth discoloration |
Although alcohol doesn’t reduce the effectiveness of most antibiotics, it can reduce energy and delay recovery from illness. So, patients should avoid alcohol until the therapy with antibiotics is finished.
How long does Amoxicillin last in the body
Orally administered Amoxicillin capsules of 250 mg and 500 mg exhibit maximal concentrations in blood 1 to 2 hours after administration. About 60% of Amoxicillin oral dose is excreted in the urine after 6 to 8 hours.
It can be detectable in serum up to 8 hours after an orally administered dose. So, if patient is planing to consume alcohol while using amoxicillin, the best way to avoid any interaction is to take amoxicillin on empty stomach and wait 8-10 hours after administration.
However, patients have to keep their alcohol intake to the minimum when they are taking antibiotics.
How long does Alcohol last in the body?
Alcohol leaves the body system in two ways:
- 10% of alcohol is eliminated through the urine, breath and perspiration
- 90% of alcohol is metabolized, broken apart in the body
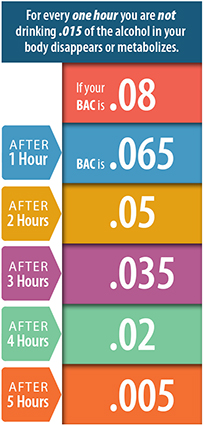
Almost everyone, independently of age, weight, or race, metabolizes alcohol at the same pace. The pace is 0.015 per hour of unit known as BAS -blood alcohol concentration.
It means that for every hour you are not drinking, 0.015 of the alcohol in your bloodstream is metabolized and eliminated from your body. So, if your BAC was 0.08 (about 3-4 beers drank in hour) it would take about 5.33 hours for the alcohol to be metabolized and eliminated from your body.
However, if someone is binge drinking, they could get into a situation where alcohol remains in their body for 10 hours or more. So, if someone planing to take amoxicillin or any other antibiotic,suggestion is to wait 8-12 hours after alcohol is being taken.
Taking Amoxicillin 500 mg with beer
What is “Disulfiram-like Reaction”? Can Amoxicilin cause this reaction?
As a penicillin based antibiotic, Amoxicillin does not cause this reaction. But some other antibiotics may cause.
The disulfiram-ethanol reaction is caused by increased acetaldehyde concentrations in plasma which are produced through the metabolism of ethanol by liver enzyme called alcohol dehydrogenase.
In normal cases, acetaldehyde is eliminated rapidly by its metabolism to acetate through aldehyde dehydrogenase metabolic reactions.
But, when Disulfiram or disulfiram structurally similar are taken, this enzyme is blocked and oxidation of acetaldehyde is irreversibly inhibited causing increased acetaldehyde concentrations in blood after alcohol consumption.
The discomfort associated with this reaction can be very unpleasant causing: severe flushing, nausea, stomach cramps, headaches, vomiting, rapid heart rate, and difficulty breathing that may be accompanied with hypotension and this reaction can be severe enough to cause death.
Which drugs can cause “Disulfiram-like Reaction”?
- Antibiotics like Metronidazol, and in some rare cases Bactrim
- Cephalosporins such as: Cefamandole, Cefoperazone, Cefotetan
- Sulphonylureas first generation drugs: Tolbutamide and Chlorpropamide
- Antifungal drug Griseofulvin
- Antiprotozoal drug Tinidazole
Factors that may increase the risk of Alcohol and Antibiotic interaction
There are many factors that can induce the intensity and speed of alcohol/drug interactions in our body. These include the patient’s age, sex, weight, and race; the absence or presents of food in the stomach; and alcohol history intake.
For example, studies have found that the levels of alcohol dehydrogenase, enzyme that metabolizes alcohol to acetaldehyde, are lower in women than in men; lower in alcoholics than in nonalcoholics and lower in Asians than in Western Caucasians.
Elderly patients are higher risk of alcohol/drug interactions compared to younger adults, because they often take more prescription drugs, they are also more likely to have a serious illness, and show age-related variations in the absorption and elimination of certain drugs.
Food generally slows the rate of alcohol absorption. Consequently, medications that increase the rate of gastric emptying, such as erythromycin or cisapride enhance the alcohol metabolism rate.
“Can you drink alcohol while taking Zyrtec?“
“What happens if you take Claritin with alcohol?“
“Is it safe to take aleve after drinking alcohol?“
“How long does alcohol stay in your system for a probation drug test?“
“Can flonase and nasacort be used together?“
“Review of metformin and glyburide in the management of gestational diabetes“