Contents
- What is Nexplanon?
- What is the mechanism of action of Nexplanon?
- What is the pharmacokinetics of the Nexplanon implant?
- Is Nexplanon an intra-uterine device (IUD)?
- How big is Nexplanon?
- How do Nexplanon works?
- How soon after Nnexplanon insertion is it effective?
- How should I replace Nexplanon?
- What are the contraindications of Nexplanon implant?
- What are the complications associated with insertion of Nexplanon implant?
- Can I get the Nnexplanon removed early?
- How much does it cost to get your Nexplanon removed?
- Will Nexplanon affect my periods?
- Can you smoke cigarettes while on Nexplanon?
- Can you drink alcohol while on nexplanon?
- What are the side effects associated with Nexplanon?
- What are the possible risks of using Nexplanon?
- Can ectopic pregnancy be a risk of using Nexplanon?
- Can ovarian cysts be caused by Nexplanon?
- Can breast cancer be caused by Nexplanon?
- Can serious blood clots be formed by using Nexplanon?
- What are some other risks that may be associated with Nexplanon use?
- When should I call my healthcare provider?
- What if I become pregnant while using Nexplanon?
- Can I use Nexplanon when I am breastfeeding?
- Who should not use Nexplanon?
- Can Nexplanon implant be implanted in patients with hypertension?
What is Nexplanon?
Nexplanon (etonogestrel) is a hormone implant that prevents ovulation. Ovulation is a process of release of an egg from an ovary. Nexplanon contains the etonogestrel which is a medication that causes changes in the cervical mucus and uterine lining of your uterus. This process makes it harder for sperm to reach the uterus and harder for a fertilized egg to attach to the uterus. In order to prevent pregnancy, Nexplanon is used as a radio-opaque implant used for contraception.

Nexplanon contains etonogestrel, which is present in a small plastic rod that is implemented into the skin of your upper arm. The drug is released slowly into the body. Nexplanon is an implant that provides continuous contraception for up to 3 years and can remain in place for 3 years. This implant contains barium sulfate in small quantities which can be seen by X-ray.
What is the mechanism of action of Nexplanon?
The Etonogestrel diffuses into the surrounding tissues from the implant that result in low circulating levels of Progestin. The Nexplanon implant releases 60 mcg of etonogestrel initially and around 30 mcg after 2 years of use. The reduced levels of the progestin thicken and decrease the amount of cervical mucus, that forms a barrier to the sperm and which suppresses the ovulation for at least 2.5 years.
The Nexplanon implant is one of the most effective forms of contraception available nowadays. It was reported to not to cause any pregnancies in a huge number of women seeking for the effective and long-lasting mode of contraception.
The Nexplanon insertion should be very accurate and the failure has been reported with implants mainly due to incorrect insertion or if it is inserted after pregnancy had already occurred. This method is so successful because it does not need any effort on the part of the user after insertion.
As per studies, Nexplanon implant is beneficial in preventing the pregnancy effectively. Nexplanon is known to reduce pregnancy rate as 1 pregnancy per 100 women when used for a year. And if it is placed correctly, the chances of getting pregnant are very low. The studies of the Nexplanon have not been done on overweight women, therefore, the efficacy is not very well known in overweight women.
What is the pharmacokinetics of the Nexplanon implant?
Absorption:
Etonogestrel is released into circulation and almost 100% bioavailable after subdermal insertion of the etonogestrel implant. As per studies based on clinical trials, Nexplanon yield comparable systemic exposure to etonogestrel. After insertion, the mean serum etonogestrel maximum level was 1200 pg/ml that achieved within 2 weeks of insertion of the Nexplanon implant.
The serum etonogestrel level decrease gradually with time and reduced up to 202 pg/ml after one year and 164 pg/ml after two years, and remain 136 pg/ml at three years.
Distribution:
201 liters is the apparent volume of distribution. Etonogestrel is approximately 32% bound to sex hormone binding globulin (SHBG) and 66% bound to albumin in blood.
Metabolism:
The etonogestrel is metabolized by the cytochrome P450 3A4 isoenzyme, in liver microsomes. The biological activity of etonogestrel metabolite is unknown.
Excretion:
The elimination half-life of etonogestrel is about 25 hours. The metabolites of etonogestrel either as free steroid or as conjugates are excreted primarily in urine and to a lesser extent in feces. The concentrations of the etonogestrel decreased below sensitivity of the assay by one week after removal of the implant.
Is Nexplanon an intra-uterine device (IUD)?
Nexplanon is placed in your arm, not in uterus, therefore, it is not an intra-uterine device. It is a long-acting birth control that lasts for up to 3 years. Nexplanon implant is a great option for contraception for women who want something long-lasting, just like an intra-uterine device (IUD). It is also a superb choice because of its low-maintenance in the day-to-day than the pill.
How big is Nexplanon?
Nexplanon consists of a single rod made of ethylene vinyl acetate copolymer that is 4 cm long and 2 mm in diameter. It is similar to a matchstick in size. The rod contains 68 mg of etonogestrel (sometimes called 3-keto-destrogestrel), a type of progestin.
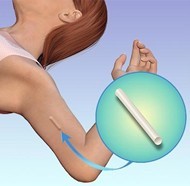
How do Nexplanon works?
Nexplanon prevents pregnancy in several ways.
- It stops the egg from being released by the ovary.
- It prevents sperm from reaching the egg.
- It thickens the mucus in your cervix which keeps sperm from reaching the egg.
- It is helpful in changing the lining of your uterus.
Nexplanon releases low dose of hormone in your blood stream. It works for 3 years and prevent pregnancy without any maintenance. Nexplanon is placed on the inner arm and upper arm.
How soon after Nnexplanon insertion is it effective?
If women get Nexplanon during the first 5 days of her period, she is then protected from pregnancy right away. If she gets the implant at any other time in her cycle, she should use some other form of birth control (like condoms) during the first week.
After that first week, the implant starts working and she is protected from pregnancy for up to 4 years. That’s why it’s called get-it-and-forget-it birth control.
How should I replace Nexplanon?
After the removal of the previous implant, immediate replacement of Nexplanon can be done. The replacement procedure is exactly similar to the insertion of Nexplanon.
In the same arm, the new implant should be done, through the same incision from which the previous implant has been done. One should anesthetize the insertion site if the same incision is being used to insert a new implant (for example, 2 mL lidocaine (1%)] applying it just under the skin along the ‘insertion canal.’).
What are the contraindications of Nexplanon implant?
Nexplanon should not be used in women who have
- Known or suspected pregnancy
- Current or past history of thrombosis or thromboembolic disorders
- Liver tumors, benign or malignant, or active liver disease
- Undiagnosed abnormal genital bleeding
- Known or suspected breast cancer, personal history of breast cancer, or other progestin-sensitive cancer, now or in the past
- Allergic reaction to any of the components of Nexplanon
What are the complications associated with insertion of Nexplanon implant?
Nexplanon implant can be felt under the skin after insertion and therefore it is inserted subdermally. The insertion of the Nexplanon is confirmed after palpation immediately after insertion. If it is not confirmed by palpation immediately after insertion, insertion of Nexplanon may go unnoticed.
Unintended pregnancy may occur due to the undetected failure of insertion. Pain, paresthesias, bleeding, hematoma, scarring or infection are some complications related to insertion and removal procedures.
The neural or vascular injury may occur if Nexplanon is inserted deeply (intramuscular or in the fascia). Nexplanon should be inserted at the inner side of the non-dominant upper arm about 3 to 4 inches in order to reduce the risk of neural or vascular injury. Nexplanon should be inserted subdermally just under the skin avoiding the sulcus (groove) between the biceps and triceps muscles.
The large blood vessels and nerves that lie there in the neurovascular bundle deeper in the subcutaneous tissue should also be avoided. Paraesthesia (due to neural injury), migration of the implant (due to intramuscular or fascial insertion), and intravascular insertion can occur due to deep insertions. One should start the suitable treatment if infection develops at the insertion site.
The implant may also need to be removed if infection persists for a longer period of time. Expulsions can also occur due to incomplete insertions or infections. The implant insertion should be accurate which means it should not be inserted too deeply, it should be palpable after insertion, It should not be encased in fibrous tissue or it should not be migrated from its place, the removal of the implant may become difficult or even impossible.
There have been reports of migration of the implant within the arm from the insertion site or within the vessels of the arm and pulmonary artery which may be related to deep insertion or intravascular insertion. Endovascular or surgical procedures may be needed for removal in case the implant has migrated to the pulmonary artery.
The implant removal or localization is recommended in case the implant cannot be palpated. Without proper identification of the location of the implant, the exploratory surgery is strongly discouraged. In order to prevent the injury to the deeper neural or vascular structures in the arm, the removal of deeply inserted implants should be done by the healthcare provider (who must be familiar with the anatomy of the arm) and that is also with extreme caution.
The healthcare provider familiar with the anatomy of the chest should be consulted in case the Nexplanon implant is inserted in the chest. Continued effects of the etonogestrel such as compromised fertility, ectopic pregnancy, or persistence or occurrence of a drug-related adverse event may be noted if the removal of the implant is failed.
Exploratory surgery without knowledge of the exact location of the implant is strongly discouraged. Removal of deeply inserted implants should be conducted with caution in order to prevent injury to deeper neural or vascular structures in the arm and be performed by healthcare providers familiar with the anatomy of the arm.
If the implant is located in the chest, healthcare providers familiar with the anatomy of the chest should be consulted. Failure to remove the implant may result in continued effects of etonogestrel, such as compromised fertility, ectopic pregnancy, or persistence or occurrence of a drug-related adverse event.
Can I get the Nnexplanon removed early?
Nexplanon can be removed at any time by during the 3-year period, but must be removed by the end of the third year. Removal involves a minor surgical procedure in which a surgeon makes a small incision in your arm where Nexplanon is located.
How much does it cost to get your Nexplanon removed?
A procedure of implant removal can cost between 200-300 USD.
Will Nexplanon affect my periods?
The normal menstrual bleeding pattern can be changed from normal menstrual bleeding pattern after starting the Nexplanon implant. These may include changes in bleeding frequency (absent, less, more frequent or continuous), intensity (reduced or increased) or duration. Implanon, a non-radio-opaque implant, the bleeding pattern can be varied.
Such as it can cause amenorrhea to frequent or prolonged bleeding in almost 1 in 5 women. The bleeding pattern experienced during the first three months of Nexplanon use is broadly predictive of the future bleeding pattern for many women. Women may undergo varied bleeding patterns therefore, they should be counseled
In clinical trials of the non-radiopaque etonogestrel implant (IMPLANON), bleeding patterns ranged from amenorrhea (1 in 5 women) to frequent and/or prolonged bleeding (1 in 5 women).
Women should be counseled regarding the bleeding pattern changes they may experience so that they know what to expect. Abnormal bleeding should be evaluated as needed to exclude pathologic conditions or pregnancy.
Can you smoke cigarettes while on Nexplanon?
There should be no significant effects/interactions between Nexplanon and smoking (although smoking is not recommended).
Can you drink alcohol while on nexplanon?
Alcohol, like etonogestrel, can alter mood and cause dizziness, nausea, and stomach pain. Drinking while an Implanon is in place can make these symptoms worse. Limit or avoid drinking while you have the implant.
What are the side effects associated with Nexplanon?
If you have signs of allergic reaction to Nexplanon, such as hives, difficulty breathing, swelling of the face, lips, tongue, or throat, call your doctor right away.
Other side effects that you should consider are:
- Redness, swelling or oozing at the site of insertion of implant
- Cramping or pain in your pelvic area (on one side especially)
- Sudden numbness or weakness, severe headache, slurred speech, vision problem or balance (these are signs of a stroke)
- Sudden vision loss, severe chest pain, shortness of breath, nausea, sweating mainly known as symptoms of a blood clot
- Heart attack symptoms such as chest pressure or pain, pain spreading to your jaw or shoulder, nausea and sweating.
- Hypertension or high blood pressure, severe headache, blurred vision, pounding in your neck or ears.
- Symptoms of depression such as sleep problems, weakness, tired feeling, and mood changes
- Swelling in your hands, ankles, or feet
- Jaundice (yellowing of the skin or eyes)
- A breast lump
What are the possible risks of using Nexplanon?
Due to a failed insertion, the implant may not be placed in your arm at all. You may become pregnant if this happens to you. You must be able to feel the insertion under the skin, immediately after insertion, with the help of your healthcare provider. If you can’t feel the implant, tell your healthcare provider.
The implant is not at the place where it should be, therefore location and removal of the implant may be difficult or impossible. The effects of Nexplanon will continue for a longer period of time if it is not removed on time. Implants may have been found in a blood vessel in the lung (also called pulmonary artery).
Your doctor may use an X-ray (or chest) or other imaging methods in order to find the implant if it is not found in the arm. Surgery may be needed if the implant is located in the chest.
Other problems related to insertion and removal is:
- Pain, irritation, swelling along with bruising at the insertion site
- Scarring, including a thick scar, called a keloid around the insertion site
- Infection
- Scar tissue may form around the implant making it difficult to remove
- The implant may come out by itself. You may become pregnant if the implant comes out by itself. Use a back-up birth control method and call your healthcare provider right away if the implant comes out.
- The need for surgery in the hospital to remove the implant
- Injury to nerves or blood vessels in your arm
- The implant breaks making removal difficult
Can ectopic pregnancy be a risk of using Nexplanon?
If you become pregnant while using Nexplanon, you have a slightly higher chance that the pregnancy will be ectopic (occurring outside the womb) than do women who do not use birth control. Unusual vaginal bleeding or lower stomach (abdominal) pain may be a sign of ectopic pregnancy.
Ectopic pregnancy is a medical emergency that often requires surgery. Ectopic pregnancies can cause serious internal bleeding, infertility, and even death. Call your healthcare provider right away if you think you are pregnant or have unexplained lower stomach (abdominal) pain.
Can ovarian cysts be caused by Nexplanon?
Nexplanon usage can also lead to the development of cysts on the ovaries; however, they usually go away without any treatment. Sometimes surgery may be needed to remove them.
Can breast cancer be caused by Nexplanon?
The occurrence of breast cancer in women using Nexplanon is not known. Avoid using Nexplanon, if you have breast cancer, or have a history of breast cancer as some breast cancers are sensitive to hormones.
Can serious blood clots be formed by using Nexplanon?
The risk of increasing blood clots can be increased by using Nexplanon, mainly if you have other risk factors such as smoking. A blood clot in the heart can cause a heart attack or a stroke, and one can also die from blood clots.
Some examples of serious blood clots are blood clots in the:
- Legs (deep vein thrombosis)
- Lungs (pulmonary embolism)
- Brain (stroke)
- Heart (heart attack)
- Eyes (total or partial blindness)
The women who smoke are at greater risk of serious blood clots. You should quit smoke, if you want to use Nexplanon. In this, your healthcare provider will be able to help you.
You should tell your healthcare provider, that you are going to have surgery or need to be on rest at least 4 weeks before. During surgery or bed rest, your chances of getting blood clots get increased.
What are some other risks that may be associated with Nexplanon use?
A few women who use birth control that contains hormones may get:
- High blood pressure
- Gallbladder problems
- Rare cancerous or noncancerous liver tumors
When should I call my healthcare provider?
Call your healthcare provider right away if you have:
- Pain in your lower leg that does not go away
- Severe chest pain or heaviness in the chest
- Sudden shortness of breath, sharp chest pain, or coughing blood
- Symptoms of a severe allergic reaction, such as swollen face, tongue or throat; trouble breathing or swallowing
- Sudden severe headache unlike your usual headaches
- Weakness or numbness in your arm, leg, or trouble speaking
- Sudden partial or complete blindness
- Yellowing of your skin or whites of your eyes, especially with fever, tiredness, loss of appetite, , dark-colored urine, or light-colored bowel movements
- Severe pain, swelling, or tenderness in the lower stomach (abdomen)
- Lump in your breast
- Problems sleeping, lack of energy, tiredness, or you feel very sad
- Heavy menstrual bleeding
What if I become pregnant while using Nexplanon?
If you think you may be pregnant, you should see your healthcare provider right away. It is important to remove the implant and make sure that the pregnancy is not ectopic (occurring outside the womb). Nexplanon is not likely to cause birth defects; the information is based on experience with other hormonal contraceptives.
Can I use Nexplanon when I am breastfeeding?
You may use Nexplanon if 4 weeks have passed since you had your baby, if you are breastfeeding your child. Etonogestrel which is present in Nexplanon implant passes into the breast milk in smaller quantities. There were no effects on growth and development for almost 3 years, reported in children who had their mother’s feed. You should talk to your healthcare provider, if you are breastfeeding your baby and want to use Nexplanon.
Who should not use Nexplanon?
Do not use Nexplanon if:
- You are already pregnant or you think you may be pregnant.
- You are suffering from conditions like deep venous thrombosis (blood clots in your legs), pulmonary embolism (blood clots in your lungs), total or partial blindness, heart diseases, or ever had a heart attack, or brain stroke.
- You have any liver disease or a lover tumor.
- You had a vaginal bleeding of unknown cause.
- You have any type of cancer (especially breast cancer) which is sensitive to progestin previously or presently.
- You are allergic to Nexplanon (etonogestrel)
Tell your healthcare provider if you have or have had any of the conditions listed above. Your healthcare provider can suggest a different method of birth control.
In addition, talk to your healthcare provider about using Nexplanon if you have conditions like diabetes, high cholesterol, headaches or migraines, kidney problems (including gallbladder), history of depression, blood pressure related problems. Your doctor should also know if you have allergies to medicines such as anesthetics or antiseptics because such medicines are used at the time of insertion or removal of the Nexplanon implant.
Can Nexplanon implant be implanted in patients with hypertension?
The hormones such as estrogen and progestogens may cause fluid retention. The chances of increasing the fluid retention are more when given in high doses or for prolonged periods. The patients, who have problems with excess fluid, should use this therapy with extra caution.
The patient with conditions like asthma, epilepsy, migraine, and cardiovascular or renal dysfunction (conditions that may adversely affected by the liquid accumulation), should be observed for exacerbation of their condition during estrogen therapy.
“How long does Plan B stay in your system after taking it?”
“What is meloxicam and what is it used to treat?“